Pancreatitis is diagnosed and treated by the GI Division of Premier Medical Group.
Pancreatitis is diagnosed and treated by the GI Division of Premier Medical Group.
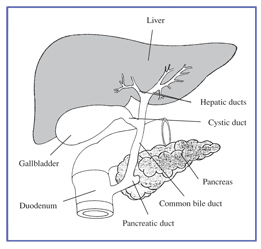
Pancreatitis is inflammation of the pancreas. The pancreas is located behind the stomach and near to the duodenum. The job of the pancreas is to help in the digestion of food by providing enzymes to mix with food. The pancreas also produces the hormones insulin and glucagon into the bloodstream which help to regulate the glucose from food for energy. Normally these enzymes become active only after they reach the small intestine, where they are necessary to digest food. If the enzymes become active inside the pancreas they eat and digest the tissue of the pancreas, causing swelling and bleeding which damages the pancreas and its blood vessels—this is called pancreatic inflammation.
Pancreatitis can be acute or chronic; both types are considered serious and can lead to complications. Bleeding, infection, and even permanent damage to the tissue may occur. Acute pancreatitis tends to affect more men than women, and rarely affects children.
The most common cause for acute pancreatitis is high alcohol intake. In some cases genetics can play a factor, as well as certain surgeries, diseases, or habits.
Other causes include:
The main symptom of pancreatitis is pain in the upper left abdomen or middle of the abdomen, which often radiates through to the back. The pain may become worse after eating or drinking, particularly if the food has a high fat content. It can also be worse when lying down flat on your back and can become more severe, lasting for a few days. Some patients complain of pain in their back or below the left shoulder as well.
Acute pancreatitis is inflammation of the pancreas that occurs suddenly. A person with acute pancreatitis generally looks and feels very ill and needs immediate medical attention.
The most common causes of acute pancreatitis are excessive alcohol intake and gallstones. After alcohol use, the symptoms can appear within a few hours, or could take several days. Other causes of acute pancreatitis include abdominal trauma, medications, infections, tumors, and genetic abnormalities of the pancreas.
Symptoms usually begin with a gradual or sudden pain in the upper left or middle abdomen, sometimes extending to the back. This pain can be mild in the start and worse especially after eating, gradually getting more constant and lasting for several days. Other symptoms can include, fever, rapid pulse, nausea and/or vomiting, and swollen and tender abdomen. Other common symptoms can include:
The pain:
Acute pancreatitis generally goes away by itself in a few days, with no treatment, but it can be life-threatening as well. In fact, each year approximately 210,000 Americans are admitted to hospitals with the disease. If the acute pancreatitis becomes severe, it may cause dehydration and low blood pressure. The heart, lungs, or kidneys can fail. If bleeding occurs in the pancreas, shock and even death may follow.
Chronic pancreatitis is an inflammation of the pancreas that does not heal over time. It just gets worse over time and leads to permanent damage. This type of pancreatitis frequently develops in people who are between the ages of 30 and 40.
The causes are the same as for acute pancreatitis, causing incidents of the same type of pain. The main cause for chronic pancreatitis is years of heavy alcohol use. This can be caused by one acute attack that damages the pancreatic duct. Some people with chronic pancreatitis show no symptoms, while others undergo abdominal pain, sometimes spreading to the back. These symptoms can become aggravated after eating or drinking, making the pain worse. Some patients report no pain after a while, but this could be because the pancreas has stopped making digestive enzymes.
Other common symptoms of chronic pancreatitis are:
Chronic pancreatitis, like acute pancreatitis, occurs when digestive enzymes attack the pancreas and nearby tissues, causing episodes of pain. The most common cause of chronic pancreatitis is many years of heavy alcohol use. The chronic form of pancreatitis can be triggered by one acute attack that damages the pancreatic duct. The damaged duct causes the pancreas to become inflamed, causing scar tissue to develop—eventually the pancreas is destroyed. Other common causes for chronic pancreatitis include:
Your doctor will first want to complete a medical history and conduct a thorough physical examination. Blood tests may be ordered to assist in the diagnosis, because with chronic pancreatitis there is an abnormal amount of lipase and amylase in the blood. Other chemical changes may also show up such as atypical glucose, calcium, magnesium, sodium, potassium, and bicarbonate. When the disease improves, these levels can return to normal.
The following are diagnostic tests used to diagnose chronic pancreatitis:
Typically acute pancreatitis requires the patient to be admitted to the hospital for several days for IV fluids, antibiotics, and pain relief. This allows the pancreas to rest while the patient does not eat or drink. Should vomiting occur, a nasal tube will be inserted to remove fluid and air from the stomach. Symptoms should improve within a few days and the patient can return home with instructions not to smoke, drink alcohol, or eat fatty foods. In the case of complications, the patient may need nasogastric feeding. This feeds a special liquid through the nose while the pancreas heals.
Depending on the severity and symptoms of the chronic pancreatitis patient, he or she may require hospitalization for pain management, IV hydration, and nutritional support.
Chronic pancreatitis requires the patient to eat a healthy low-fat diet, drinking lots of fluids, limiting caffeine, eating small frequent meals, and making sure you have enough calcium and vitamins in your diet. You may be prescribed pancreatic enzymes, which are taken at each meal. People with chronic pancreatitis (and acute pancreatitis) should avoid alcohol and smoking.
Your doctor may prescribe pain medicines or even a surgical block for pain relief. Some patients take insulin to control glucose levels. In very severe cases, part or all of the pancreas may be removed.
Pain in the upper left abdomen can be caused by things besides pancreatitis. Many of these conditions are quite serious or even life-threatening. Any pain that is out of the ordinary should be checked out by a doctor, but especially pain in the upper left abdomen. Don’t try to diagnose yourself. Often, even doctors will need to order tests to make a confident diagnosis. Here are the most common causes of upper left abdominal pain.
Heart/Cardio
These are some of the most serious causes of pain in the upper left abdomen. As with acute pancreatitis, they require immediate medical attention. They also underscore the importance of not ignoring upper abdominal pain, especially when it’s on the left side.
Digestive/Gastro-Intestinal
There a handful of issues with the upper GI system that can mimic the upper left abdominal pain of heart issues or pancreatitis. While these problems are rarely life-threatening, they can still be quite painful. Treatments are available.
Respiratory/Lungs
Among the numerous conditions that can afflict the respiratory system, there are a few that are more likely to cause pain in the upper left abdomen. This could be an infection in the left, right, or both lungs (pneumonia), inflammation of the membrane inside the chest wall (pleurisy), or trapped air threatening to collapse the lung.
Chest, Ribs, and Back
Along with muscle strains and pinched nerves, there are a couple conditions that can cause upper abdominal pain above and beyond a person’s normal amount of aches and pains. The cartilage that connects the rib cage with the breastbone can become inflamed as with costochondritis. Broken ribs or other physical trauma may also cause pain in this area.
Other Organ-Related Conditions
Pain that radiates through the back can be an apt description of pancreatitis—as well as kidney stones. Appendicitis often causes pain which gravitates to the lower right abdomen as the condition progresses, but the pain may start in the upper abdomen. In general, abdominal pain can be a surprisingly tricky thing to describe and locate, but a conversation with your doctor combined with a physical exam can determine the likely cause of the pain and whether follow-up testing is warranted.
