Fourteen years ago, when Bob (not his real name) and his wife decided not to have any more children, Bob had a vasectomy. The couple eventually divorced, Bob recently
remarried, and he and his new wife wanted to start a family together. Bob had heard about vasectomy reversal (VR) and contacted Premier Medical Group’s Dr. Jason Krumholtz, the only urologist to have performed VR at one of our regional hospitals. “He explained everything, from start to finish, very clearly,” says Bob, who had the procedure in September 2014 and reports excellent results.
“About 6 percent of patients who undergo vasectomy will, at some point, decide to have it reversed,” Dr. Krumholtz says. There are two options for patients who have had a vasectomy and want to biologically father a child: microsurgical vasectomy reversal or in vitro fertilization with testicular or epididymal sperm extraction. “But the advantage of vasectomy reversal,” says Krumholtz, “is that it is significantly less costly and avoids some of the risks of IVF, gives the couple the opportunity to have a spontaneous pregnancy, and in many situations carries a higher success rate than IVF.”
“The greatest success is achieved the closer the reversal procedure is to the vasectomy,” he says. If the interval is less than 3 years, achievable patency is 97 percent, at 3 to 8 years it is 88 percent, at 9 to 14 years it’s 79 percent, and for 15 years or more, the rate is 71 percent. Pregnancy rates are largely affected by the spouse’s age.
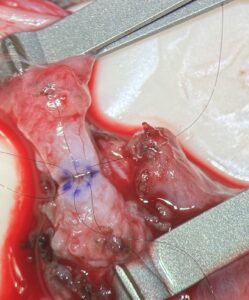
In a vasectomy, the vas deferens, or sperm duct, is cut to prevent sperm from reaching the ejaculate fluid. In VR the ends of the severed vas deferens are microsurgially reconnected in a procedure known as vasovasostomy. With the patient under general anesthesia, a small incision is made on each side of the scrotum and the scarred ends of the vas are removed. Fluid is sampled from the end closest to the testicle and viewed in the operating room with a light microscope to see if it contains sperm. Using a large high-powered operative microscope, each end of the vas deferens is then microsurgically reattached. Dr. Krumholtz prefers what is commonly referred to as a two layered technique: The lumen or channel inside the vas deferens is circumferentially reapproximated with 6-8 individual 10-0 nylon microsutures. Then a second layer, the seromuscular layer, is reapproximated with stronger 9-0 nylon microsutures. In addition, if necessary, the periadvential layer, a third layer, is used to strengthen the anastomosis.
“The lumen of the vas is half a millimeter in diameter, and the whole vas is the diameter of a piece of spaghetti,” says Dr. Krumholtz. “Furthermore, each end of the vas deferens is not identical in size. The end closest to the testicle is often larger, sometimes significantly so, than the end closest to the abdomen. This, along with the use of suture that is not visible without the aide of the operative microscope, can make the surgery technically demanding.” At Vassar Brothers Medical Center, Dr. Krumholtz uses the same team of highly skilled nurses and technicians to assist in the surgery. Says Krumholtz, “This procedure is really a team effort. It simply wouldn’t be possible without the aide of a consistent, dedicated, knowledgeable, and skilled crew which I am very grateful to have at Vassar.”
VR takes two to three hours per side, and is done on an outpatient basis. Recovery is similar to that for vasectomy. “There is a recuperation period, and patients frequently don’t return to work for 10 to 14 days. Then, it takes three to six months to reach normal sperm counts,” Krumholtz says. Bob confirms this. “I was a bit uncomfortable after the anesthesia wore off, but had no severe pain,” he says. “The first week I was sore, and I was out of work for two weeks, but since then, no problems.” Now, his sperm count and motility are 100 percent normal. “I would recommend this surgery and Dr. Krumholtz,” he says.
