Minimizing the Side Effects of Prostate Cancer Radiation Therapy.
Optimizing your Quality of Life.
Premier Medical Group has added a new technology for men choosing to undergo radiation therapy for prostate cancer. The new addition, SpaceOAR hydrogel, is a protective spacer between the prostate and the rectum. It has been clinically proven to reduce the risk of side effects during and after radiation treatment.
If you or a loved one has been diagnosed with prostate cancer, you may be considering radiation therapy for treatment. Radiation therapy is extremely effective in targeting and treating prostate cancer, but as with any procedure there are potential side effects. These side effects can be mild and go away on their own, but for some patients they can last for years after treatment is completed and can have a profoundly negative impact on quality of life. Side effects can include:
• Rectal pain and bleeding
• Chronic diarrhea
• Urinary urgency and leakage
• Erectile dysfunction
What is SpaceOAR® hydrogel?
SpaceOAR hydrogel is an absorbable hydrogel that temporarily creates space between the prostate and the rectum, protecting the rectum from radiation exposure during prostate radiation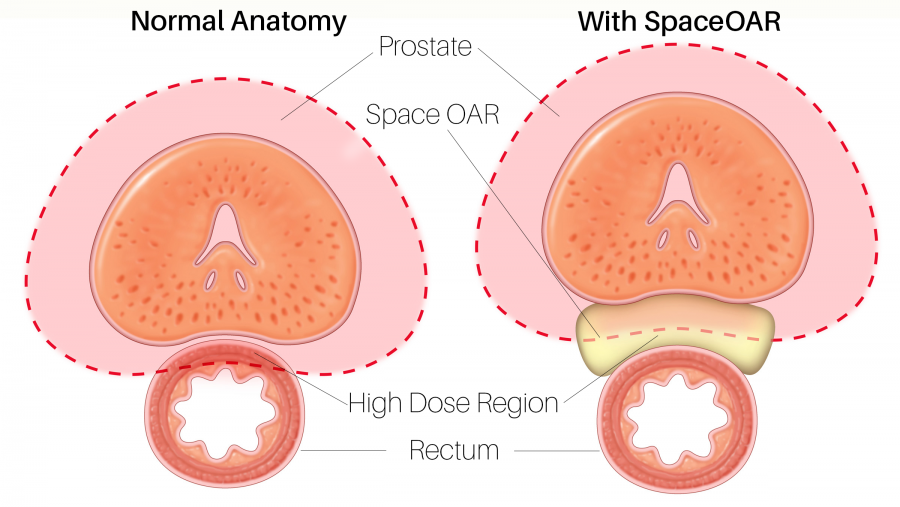 therapy.
therapy.
Why should I have SpaceOAR hydrogel?
The goal of radiation therapy to treat prostate cancer is to maximize the radiation dose to the prostate to kill the cancer cells while avoiding radiating surrounding normal tissue. Rectal injury can occur because the rectum sits next to the prostate and can accidentally receive high radiation doses and damage to healthy tissue can cause side effects. The “OAR” in SpaceOAR stands for “Organ At Risk”, and with Radiation Therapy to the prostate, this organ is the rectum.
How will SpaceOAR hydrogel help me?
By acting as a spacer, the hydrogel pushes the rectum a ½ inch away from the prostate so damage to the rectum is reduced or even eliminated. With SpaceOAR hydrogel in place, your doctor can enhance your radiation treatment to better target your cancer while preserving healthy tissue to help ensure that your rectal, urinary and sexual quality of life will be maintained.
(The procedure cannot be used with testicular cancer treatment, but the testicle’s natural distance from the body already minimizes collateral damage to other areas of the body.)
What is it made of and is it safe?
SpaceOAR hydrogel is made up of two liquids that when combined form a soft gel material that is mostly made of water. Because of the water content it is called a hydrogel. It can be safely used in the body without causing injury or a reaction. The material that the SpaceOAR hydrogel is made from has been used in other implants such as surgical sealants used in the eye, brain and spine
Has SpaceOAR hydrogel been approved?
SpaceOAR hydrogel has FDA clearance in the US and is approved for use in Canada, Europe, Japan, Australia and other countries around the world.
In what type of radiation treatment can SpaceOAR hydrogel be used?
SpaceOAR hydrogel can be used in all types of radiation therapy. Here are the four most common types:
External radiation (or external beam radiation – EBRT) uses a machine that directs high-energy rays (or photons) from outside of the body into the tumor. Most patients get external radiation therapy over many weeks, during outpatient visits to a hospital or treatment center.
Internal radiation, also called brachytherapy, involves putting a radioactive source inside the body into or near the tumor.
Stereotactic body radiation therapy (SBRT) uses advanced imaging techniques to deliver extremely precise, very intense doses of radiation to the prostate (usually in up to five treatments over a period of days).
Proton Beam therapy uses proton particles in lieu of x-rays or photons.
Where is the procedure done and how long does it take?
SpaceOAR hydrogel can be implanted as an outpatient procedure in a hospital, surgery center, outpatient clinic or doctor’s office prior to the start of radiation treatment, and is typically not a lengthy procedure.
How is SpaceOAR hydrogel implanted (put into place)?
The SpaceOAR hydrogel is injected as liquid through a small needle between the rectum and the prostate. Your doctor will use ultrasound imaging to ensure correct placement.
Will I be awake or asleep during the procedure?
SpaceOAR hydrogel can be implanted under local, regional or general anesthesia. You should discuss with your doctor which type of anesthesia will work best for you.
What do I need to do to get ready before the procedure?
Your doctor will give you instructions on how to prepare for the procedure and information about any anesthesia you will receive.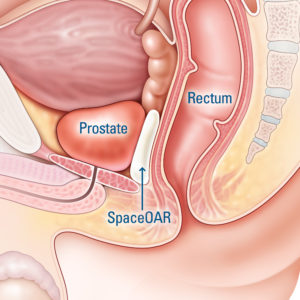
Will I feel any discomfort or pain during or after the procedure?
Your doctor will use a local, regional or general anesthesia and the injection site will be numbed, so you may feel a pinprick or pressure but should not feel any discomfort. Following the implantation, you may experience some temporary discomfort at the injection site. SpaceOAR hydrogel patients typically report no prolonged discomfort from the implanted gel.
How soon after the procedure can I return to my normal activities?
You should be able to go back to your normal activities right away. Check with your doctor about anything you should avoid after the procedure and during your
radiation treatments.
How long will SpaceOAR hydrogel remain in my body?
SpaceOAR hydrogel stays in place, separating your prostate and rectum, for about 3 months. After 6 months, the hydrogel is naturally absorbed into the body and removed in your urine.
Has SpaceOAR hydrogel been clinically tested?
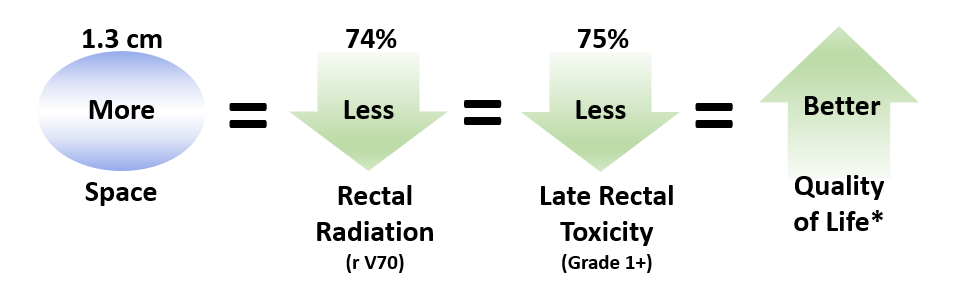
SpaceOAR hydrogel has been evaluated in many clinical studies and shown to be safe and effective in reducing side effects. In the U.S., 222 prostate cancer patients participated in a multi-center, randomized, patient-blinded clinical study. Study results showed that the hydrogel was safe and effective. The average SpaceOAR hydrogel study patient gained ½ inch of space between the prostate and rectum, and had significant reduction in radiation dose to the rectum resulting in significantly fewer rectal side effects.
Follow-up Study
Three years after treatment, patients from the study were asked to report on their Quality of Life for bowel, urinary and sexual functions. These patient-reported outcomes showed that SpaceOAR hydrogel patients experienced significantly fewer long-term rectal side effects, were more likely to maintain sexual function, and had significantly higher patient reported scores for urinary and bowel Quality of Life.