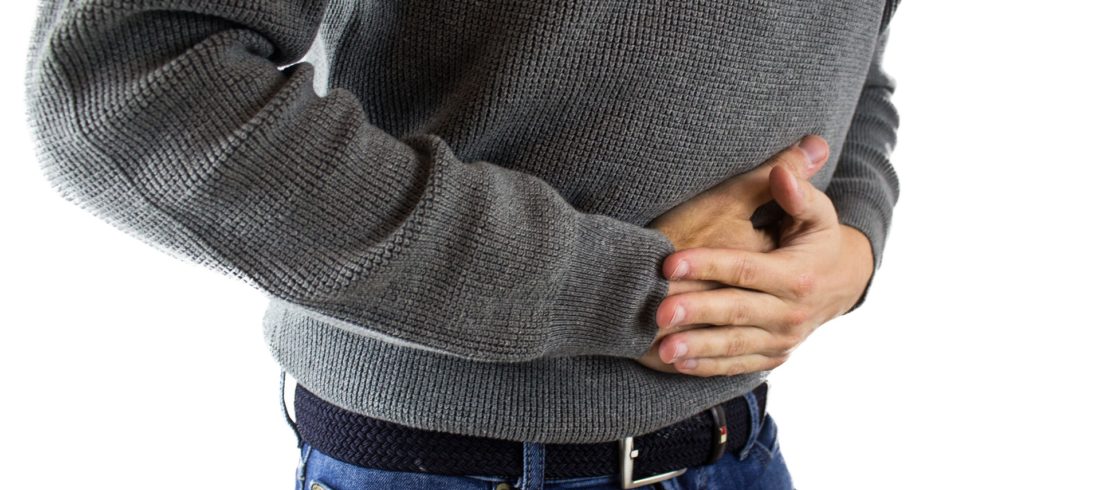
IBS and IBD – What’s the difference between?
We hear a lot about IBS and sometimes about IBD, so some people wonder, are these just different names for the same disorder? While both affect the digestive tract, the answer is no and it helps to understand the differences:
-
IBS is Irritable Bowel Syndrome
- It is uncomfortable, you may feel bloated and although it has a lot of symptoms in common with IBD, IBS is usually limited to the colon and usually does not cause lesions or ulcers in the bowel. It affects 15-20% of people worldwide.
-
IBD is Inflammatory Bowel Disease.
-
- IBD is actually a group of complex disorders including Crohn’s disease which may have an impact on any part of the gastrointestinal tract, while ulcerative colitis only affects the large and small intestine, the rectum and the anus). IBD is painful, and can cause ulcers or lesions.
There are three kinds of IBS
It is not the intention of gastroenterologists to confuse us with three kinds of irritable bowel syndrome. The idea is to help you understand what type of IBS you have. Some kinds of IBS are called IBS-D which is IBS where diarrhea is one of the most common symptoms. There is also IBS-C where constipation is among the most common symptoms. In addition there is mixed IBS, where you may experience both constipation and diarrhea.
No matter which kind you have, IBS is not life-threatening. It does, however, affect your quality of life. There is no outright cure, so the goal of treatment is to reduce symptoms as much as possible. Treatments may be focused on improving the uncomfortable symptoms of IBS-C – such as abdominal pain and bloating – or on improving bowel function.
Both IBS and IBD may have these symptoms.
- Abdominal pain
- Diarrhea
- Gas and bloating
- Abdominal cramping
- Nausea, and/or vomiting
- An urgent need for a bowel movement
- Fibromyalgia
- Urinary frequency and urgency
IBD symptoms (Crohn’s disease and ulcerative colitis)
These symptoms are unique to IBD and they are more serious:
- Anemia
- Eye redness or pain
- Feeling tired
- Fever
- Joint pain or soreness
- Skin changes
- Unintended weight loss
- Loss of appetite
- Rectal bleeding
What causes IBS?
At this moment, researchers don’t have all the answers about the causes of IBS. However, there are age characteristics – if you are over 50, you’re more likely to have it. And there is very possibly a genetic factor at work. If other members of your family have IBS, the chances are stronger that you are likely to get IBS.
Getting a confirmed diagnosis is the first important step
While there is not one simple test to tell you if you have IBS, if you think you might have it, or have a family history of IBS or gastrointestinal cancer, you should make an appointment with a gastroenterologist, who is a doctor who specializes in disorders of the digestive system. It is important to have an informed opinion to arrive at the correct diagnosis
When to get help
If you frequently experience abdominal pain or discomfort along with changed bowel habits, you may have IBS. People with IBS often report that these symptoms have been present, to some degree, for many months or years. The pain is usually described as abdominal cramps that come and go, which often improve after having a bowel movement. If you are using over-the-counter medications regularly to reduce symptoms, you should consult a doctor to determine the best course of treatment.
Some tests your gastroenterologist may order
Your doctor may recommend a number of tests to clarify your diagnosis including:
Imaging tests
- Flexible sigmoidoscopy – your doctor will examine the lower part of the colon (the sigmoid) with a flexible, lighted tube (the sigmoidoscope)
- Colonoscopy – Your doctor uses a small flexible tube to examine your entire colon
- X-Ray or CT Scan – Images of your abdomen and pelvis to help your doctor rule out other causes of your symptoms
Lab tests for IBS
- Lactose intolerance tests
- Stool tests
- Upper endoscopy– A long, flexible tube is inserted down your throat and into the tube connecting your mouth and stomach (esophagus). A camera on the end of the tube allows the doctor to inspect your upper digestive tract and obtain a tissue sample (biopsy) from your small intestine and fluid to look for overgrowth of bacteria. Your doctor might recommend endoscopy if celiac disease is suspected
- Breath test for bacterial overgrowth – Measuring the levels of hydrogen, methane and carbon dioxide in your breath can identify if you have excess bacteria in your small intestine. Bacterial overgrowth is more common among people who have had bowel surgery or who have diabetes or some other disease that slows down digestion
When you have a diagnosis of IBS, what’s next?
Once you know that you have IBS and nothing more serious, you can breathe a little easier. Then you and your gastroenterologist can focus on relieving your symptoms.
Dietary therapy- avoiding trigger foods
If you have mild IBS, lifestyle and dietary changes may control symptoms completely. Which foods cause which symptoms varies for each individual. There are no reliable tests to identify which foods may trigger symptoms, but some foods containing lactose or gluten are common problem foods for people with IBS. For those people, avoiding these foods can improve symptoms.
What about gluten and dairy?
Not every person who is sensitive to wheat and gluten- containing foods has celiac disease. In fact there is a condition that is common among IBS patients called non-celiac gluten sensitivity (NCGS). In a double-blind crossover trial 37 patients with IBS and non-celiac gluten sensitivity (NCGS) but not celiac disease improved markedly on a low FODMAP diet and became worse on diets containing gluten or whey.
Using the FODMAP diet
It is not always easy to figure out what foods may “trigger” your symptoms. In these cases, symptoms may improve with a diet low in FODMAPs (Fermentable Oligosaccharides, Disaccharides, Monosaccharides And Polyols) or foods low in a type of sugar called fructose (which is found in many types of fruit). Avoiding foods that are known to cause increased gas production, such as onions, celery, carrots, beans, prunes, wheat, alcohol or caffeine, can help.
When should I seek medical help?
If you have abdominal discomfort or symptoms that last longer than three months and include weight loss, bleeding, iron deficiency (low levels of iron based on blood tests) or symptoms that start after age 50, it’s time to see your primary care doctor or a gastroenterologist.
Tell the doctor if over the counter medications are not giving you relief. Be sure to mention if you have a family history of gastrointestinal diseases such as inflammatory bowel disease, celiac disease or cancer. If you are worried that you might have something serious, staying away from the doctor will only make it worse. Be brave. Take the first step and make an appointment, you’ll feel better and the gastroenterology group at Premier Medical Group is here to help.